A multidisciplinary approach to the treatment of malignant heart tumor
Автор: Shumakov D.V., Dudakov V.A., Zybin D.I., Vashchenko A.V., Gegenava B.B., Tereshina A.A., Ivashkin B.V., Kurnosov S.A., Kapranov M.S., Popov M.A.
Журнал: Московский хирургический журнал @mossj
Рубрика: Клинические случаи
Статья в выпуске: 4 (74), 2020 года.
Бесплатный доступ
Introduction: paragangliomas are rare neuroendocrine neoplasms with a frequency of 0.001-0.01% in population, which arise from the adrenal medulla and extrarenal autonomic paraganglia, respectively. Paragangliomas of the heart are extremely rare primary neuroendocrine tumors of the heart, accounting for less than 1% of all cardiac neoplasms. Their location is clinically important as they can interfere with heart function. For large paragangliomas of the heart with myocardial invasion, the need for heart reconstruction or transplantation may potentially arise.Discussion: in our case, taking into account the secretion of catecholamines, sick sinus syndrome, a high risk of bleeding, and tumor fragmentation, the first stage was to achieve the regression of the tumor by means of embolization of heart tumor suppliying afferent with coils. However, due to several sources of blood supply of newgrowth, this method of treatment did not lead to the desired effect. In this regard, the tactics of open surgical intervention was chosen to remove the newgrowth with the reconstruction of heart chambers. According to the data of postoperative biopsy, removed tumor was paraganglioma. Conclusion: this experience shows the importance of a multidisciplinary and personalized approach in treatment of patients in a multidisciplinary hospital.
Paraganglioma of the heart, malignant tumor of the heart, endovascular surgery, embolization of a heart tumor, cardiac surgery
Короткий адрес: https://sciup.org/142229620
IDR: 142229620 | УДК: 616.12-089.84 | DOI: 10.17238/issn2072-3180.2020.4.95-100
Текст научной статьи A multidisciplinary approach to the treatment of malignant heart tumor
Introduction: paragangliomas are rare neuroendocrine neoplasms with a frequency of 0.001–0.01% in population, which arise from the adrenal medulla and extrarenal autonomic paraganglia, respectively. Paragangliomas of the heart are extremely rare primary neuroendocrine tumors of the heart, accounting for less than 1% of all cardiac neoplasms. Their location is clinically important as they can interfere with heart function. For large paragangliomas of the heart with myocardial invasion, the need for heart reconstruction or transplantation may potentially arise.
Discussion: in our case, taking into account the secretion of catecholamines, sick sinus syndrome, a high risk of bleeding, and tumor fragmentation, the first stage was to achieve the regression of the tumor by means of embolization of heart tumor suppliying afferent with coils. However, due to several sources of blood supply of newgrowth, this method of treatment did not lead to the desired effect. In this regard, the tactics of open surgical intervention was chosen to remove the newgrowth with the reconstruction of heart chambers. According to the data of postoperative biopsy, removed tumor was paraganglioma. Conclusion: this experience shows the importance of a multidisciplinary and personalized approach in treatment of patients in a multidisciplinary hospital.
Paragangliomas are rare neuroendocrine neoplasms with a frequency of 0.001–0.01% in the general population, which arise from the adrenal medulla and extrarenal autonomic paraganglia. Paragangliomas are associated with pheochromocytoma of adrenal glands, as both are of neuroectodermal origin. Although most paragangliomas are sporadic, up to 40% of them can be associated with hereditary syndrome [1,3]. Local progression of tumor can lead to severe outcomes due to the impact of paragangliomas on surrounding structures, so surgical intervention is recommended [4].
Mediastinal paragangliomas are rare, approximately 200 cases are described in the literature and account for only 2% of all cate-cholamine-secreting tumors [4, 5].
Paraganliomas of the heart are extremely rare primary neuroendocrine tumors of the heart, accounting for less than 1% of all neoplasms of the heart [1, 2]. Their location is clinically important as they can disturb with heart function. There are other neoplasms to consider when differentiating the diagnosis, including benign tumors such as myxomas, lipomas, hamartomas, and rhabdomyomas, and malignant tumors such as sarcomas and lymphomas [1].
Excision of tumor is the main method of treatment in such patients, however, dangerous complications arise due to the removal of a part of the heart [1–5]. Caution should be exercised due to the potential oversecretion of catecholamines during surgery. One important surgical complication is bleeding, since these tumors are highly vascularized and their blood supply comes from coronary arteries [1]. The second common complication is the release of catecholamines during manipulation with the tumor, which can lead to collapse of blood circulation [1].
For large paragangliomas of the heart with myocardial invasion, the need for heart reconstruction or transplantation may potentially arise [1].
Clinical characteristics of the patient
Patient S., 47 years old, since December 2019. began to feel a rapid heartbeat with interruptions in heart rhythm, accompanied by dizziness and discomfort behind the sternum. Then he visited local polyclinics with a preliminary diagnosis: «Paroxysmal form of atrial fibrillation». Holter monitoring revealed a persistent form of atrial fibrillation-fluttering, ventricular extrasystole of class 2 according to Lown. Multispiral computed tomography revealed a thrombus in the right atrium. The patient was referred for a consultation at Moscow Regional Research and Clinical Institute («MONIKI»).
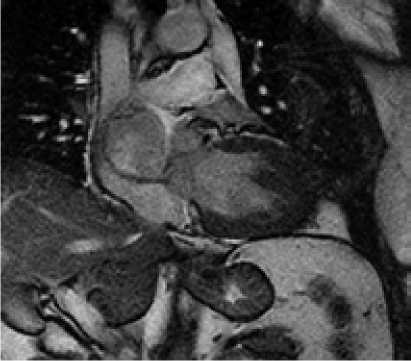
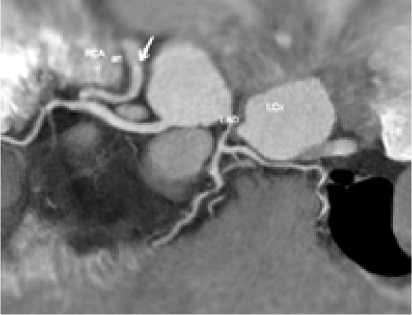
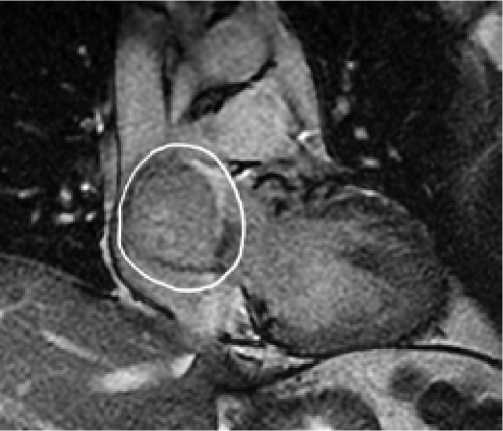
During outpatient examination and instrumental research methods, including transthoracic echocardiography (Echo-CG), magnetic resonance imaging of the heart (MRI of the heart) (Fig.
1) and multispiral computed tomography (CT) (Fig. 1), a preliminary diagnosis was made: «Hemangioma of the heart». With this diagnosis, patient was admitted to the department of cardiac surgery for adults for additional examinations and determination of treatment tactics.
C
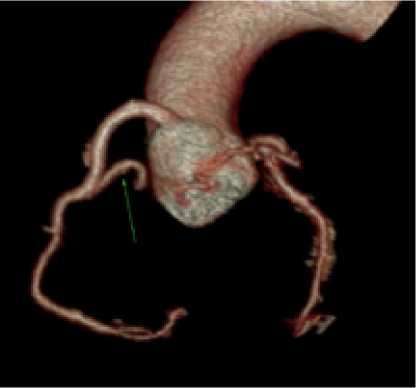
Fig. 1. Outhospital radiodiagnostics. (А) MRI of the heart, (B) MSCT of the heart; (C) 3D- reconstruction.
Electrocardiography (ECG): sinus rhythm with a heart rate of 85 beats/min; 1st degree AV block; horizontal direction of the electrical axis of the heart; RR—0.68s, PQ—0.26s, QRS—0.09s, QT — 0.30s.
Transesophageal echocardiography revealed a volumetric mass of the right atrium (67×54 mm), located high in upper and medial walls of the right atrium; blood flow is traced inside the newgrowth, compression of the superior vena cava and the right branch of the pulmonary vein is not excluded.
For diagnostic purposes and determination of further tactics, coronary angiography (CAG) was performed, which revealed a volumetric newgrowth of the right atrium, which was supplied with afferent from the right coronary artery.
Results of general and biochemical blood tests were without deviations from the norm.
Examinations confirmed the likelihood, that patient had a heart hemangioma. Heart-team decided to conduct an endovascular intervention to embolize the afferent extending from the RCA and supplying blood to the newgrowth of the right atrium.
Endovascular intervention stages
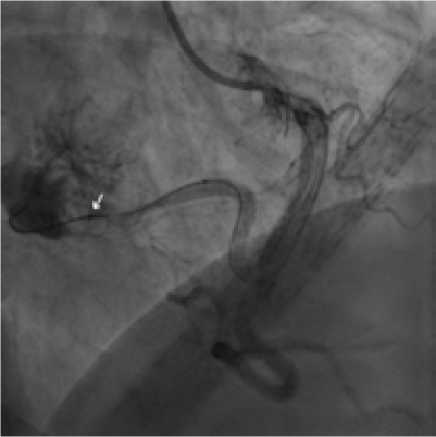
Anesthesia included premedication, local anesthesia of puncture site, and intravenous sedation with anesthesia. To perform this operation, right transradial approach was chosen. Through a 6 Fr guiding-catheter, which was placed in the entrance of right coronary artery, a coronary guidewire was inserted into distal part of the afferent, upon which the Progreat 0.021’’ microcatheter was then inserted. Then the implantation of five Hilal pushable coils was performed: two coils — 6x5 mm, three — 4x7 mm. Control angiograms showed complete occlusion of the main afferent, residual minimal contrasting of the newgrowth due to an additional smallcaliber afferent extending from the proximal third of the main afferent artery (Fig. 2).
Postoperative period
Complaints that bothered the patient before the operation, became less significant on the first day after the intervention.
ECG: sinus rhythm with heart rate 87 beats/min; 1st degree AV block; horizontal direction of the electrical axis of the heart; QRST morphology compared to the previous ECG before the intervention without significant dynamics.
Transthoracic echocardiography: a decrease in the size of the newgrowth of the right atrium.
MRI of the heart with contrast in the early postoperative period confirmed a decrease in the size of the lesion (42×43×46 mm) when compared with the previous study (46×50×47 mm) before surgery (Fig. 3).
Patient S. was discharged on the 11-th day after the endovascular operation under the supervision of a local cardiologist.
A
B
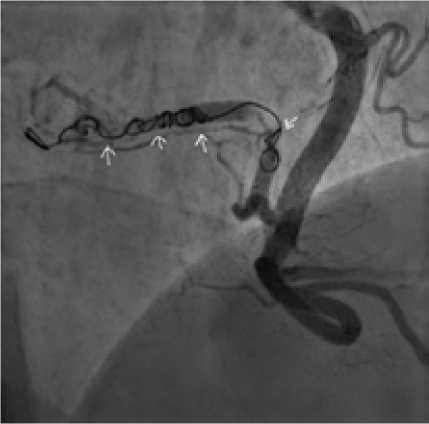
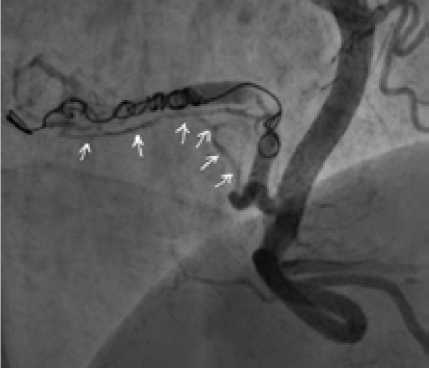
Fig. 2 . Endovascular intervention stage
B
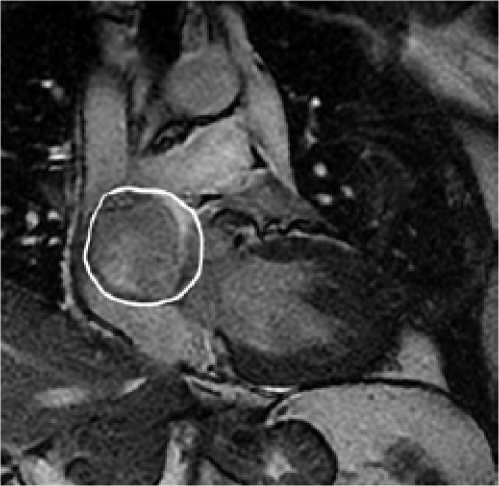
Fig. 3. MRI of the heart with contrast (a) before and (b) after tumor embolization
Patient examination after 4 months
Due to COVID-19 quarantine in the Russian Federation, hospitalization of the patient for dynamic examinations was postponed indefinitely.
After the quarantine restrictions were lifted, the patient was hospitalized with complaints on palpitations with interruptions in heart rhythm, accompanied by dizziness and discomfort in the chest.
ECG: supraventricular rhythm, tachycardia with a heart rate of 117–120 beats/min; 1st degree AV-block; horizontal direction of the electrical axis of the heart; left ventricular hypertrophy; metabolic
changes in the ventricular myocardium; RR — 0.50-0.51s, PQ — 0.26s, QRS — 0.08s, QT — 0.30s.
Transthoracic echocardiography: newgrowth of the right atrium with reduced size (34×24 mm).
Contrast-enhanced cardiac MRI: no dynamics in the reduction of lesion size in comparison with previous study in the early postoperative period (Fig. 4).
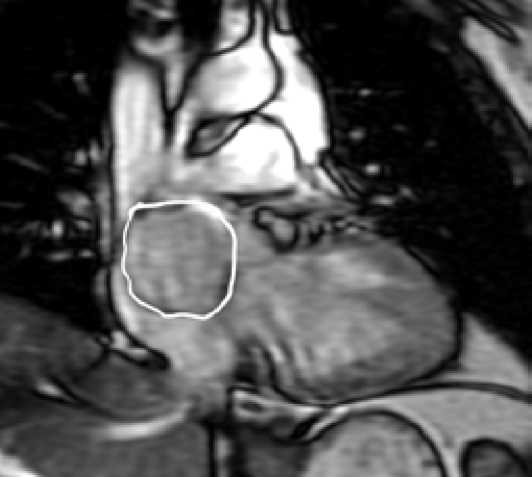
Fig. 4. MRI of the heart 4 months after tumor embolization
Angiography: right coronary artery without changes; entrance of main afferent locates in the middle segment of RCA; afferent supplies the newgrowth of the right atrium, in the lumen of it there are embolizing materials — coils slowing down the blood flow through afferent. Additional afferent with a diameter of about 2 mm and beginning locating in the proximal third of the main afferent, also supplies the newgrowth with blood flow (Fig. 5).
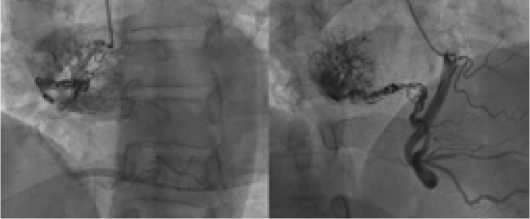
Fig. 5. Angiography: condition after endovascular embolization of the newgrowth
Later, Heart-team made a conclusion, which, due to the lack of positive dynamics in the patient’s condition, indicated a need of open surgical operation for removement and histological examination of the newgrowth.
In mid-July 2020 the patient underwent surgical intervention: removal of newgrowth of the heart with reconstruction of the roof of the left atrium, interatrial septum and wall of the right atrium with patches from the autopericardium, with use of solution of glutaraldehyde. Operation was performed using a standard sternotomy approach. After pericardiotomy, revision of the mediastinum revealed a tumor-like newgrowth in the cavity of the right atrium with a transition to the beginning of the superior vena cava and the roof of the left atrium (Fig. 6).
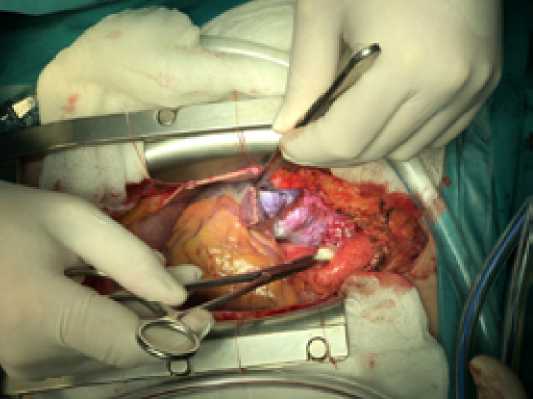
Fig. 6. Intraoperative photo of the newgrowth (between the aorta and SVC)
For ease of manipulation, the superior vena cava was skeletonized on all the way to the right venous angle. Connection of a heart-lung pump machine according to the scheme: aorta-vena cava with cannulation of the superior vena cava at the confluence of the unnamed vein. In conditions of complete cardiopulmonary bypass on the beating heart, a right atriotomia was performed with revision of the right atrial cavity: tumor invades the superior wall of the right atrium, the secondary interatrial septum with subocclusion of the superior vena cava orifice and spreads to the roof of the left atrium. It was decided to perform radical removal of the heart tumor. The branch of the right coronary artery feeding the formation was skeletonized, sutured, tied and transected. Under conditions of moderate hypothermia at 34 °C and pharmaco-cold cardioplegia with 2000 ml KUSTODIOL solution, a high-density tumor sized 5*4*4 cm, was removed in a single block within healthy tissues, with the formation of defects in the secondary interatrial septum, right atrium and left atrial roof (Fig. 7).
During removal of tumor, a branch from the circumflex artery of the left coronary artery, supplying the tumor was revealed; it was sutured and transected. Heart chambers were reconstructed with autopericardial patches pretreated with glutaraldehyde solution. The first patch was applied to the roof of the left atrium with a transition to the secondary interatrial septum, fixed with a twisted atraumatic prolene 4/0 suture (Fig. 8).
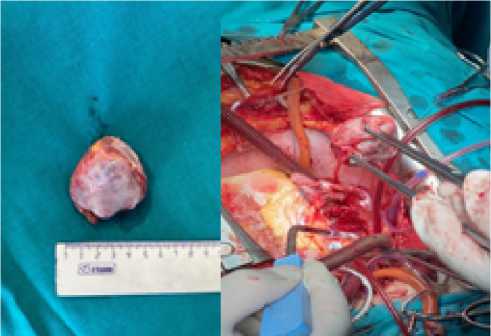
Fig. 7. Removed tumor
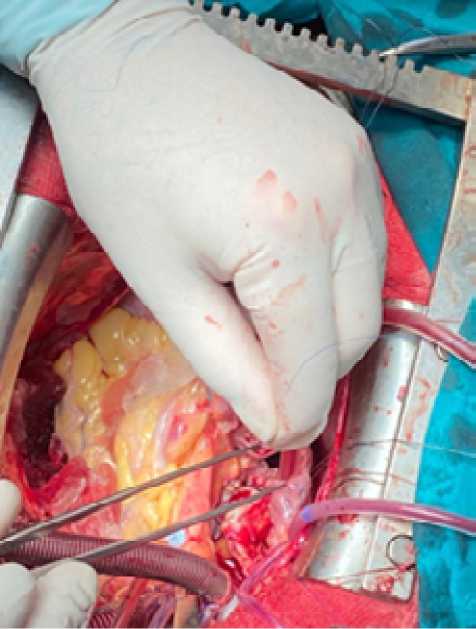
Fig. 8 . Roof patch for LP
The second patch was used to reconstruct the wall of the right atrium and the ostium of the superior vena cava, which was fixed with an atraumatic twisting suture prolene 4/0 (Fig. 9).
Restoration of cardiac activity through a single electrocardioversion. Standard completion of the operation. Artificial circulation time was 120 min, the aortic occlusion time was 95 min. The early postoperative period was satisfactory. Artificial lung ventilation — 10 hours. Sympathomimetic support—6 hours. On the second day, patient was transferred to the department of cardiac surgery for adults. Antibacterial, cardiometabolic and antiarrhythmic therapy was used.
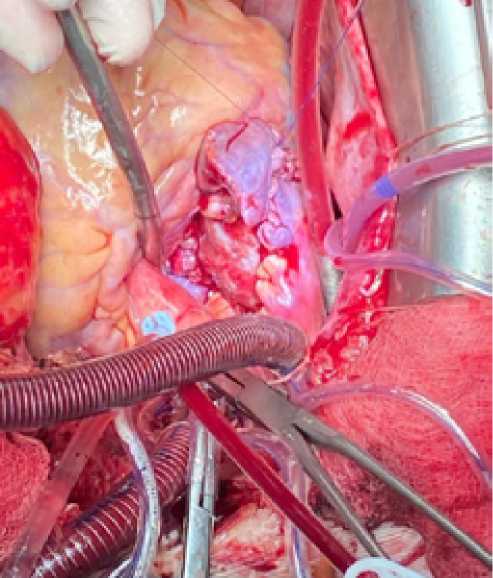
Fig. 9. Reconstruction of the right atrium
On echocardiography after removal of the newgrowth, a moderate increase in volume of right chambers of the heart was noticed. Ejection fraction was 60%. Left chambers of the heart were not dilated, moderate myocardial hypertrophy. Diastolic dysfunction type 1. No liquid was found in pericardium and pleural cavities. On the ECG, the ectopic mean right atrial rhythm with a heart rate of 80 beats/min.
After two weeks, patient was discharged in satisfactory condition.
Histological examination: a heart tumor of a solid alveolar structure with foci of necrosis, hyalinosis, edema; from large cells with rounded-oval, in places ugly nuclei, noticeable nucleoli and a finely dispersed distribution of chromatin, with a wide rim of weakly eosinophilic, vesicular and optically empty cytoplasm. Mitoses 1 in 10 RPZ (with magnification ×400). There are focal diapedesic hemorrhages, plethora of blood vessels, in lumens of large-caliber vessels - mixed thrombus with round dense amorphous basophilic masses. In the adjacent myocardium - foci of sclerosis, lipomatosis, mild lymphoplasma cell infiltration.
For the differential diagnosis between paraganglioma and large cell neuroendocrine tumor, an immunohistochemistry (IHC) study was performed.
Results of the IHC study: tumor cells express neuroendocrine markers — synptophysin and chromogranin A, in some foci — vimentin and do not express broad-spectrum cytokeratins (clone AE1/AE3), as well as somatostatin type 2 and type 5 receptors.
The proliferative activity of cells in the tumor tissue is expressed unevenly: the average Ki index 67 in the areas of maximum proliferative activity is 9.8%, in areas of minimum proliferative activity it is 2–3%. Conclusion: features of the histological structure and immunophenotype of tumor cells refers to paraganglioma.
DISCUSSION
Clinical picture of paragangliomas of the heart varies depending on the location and secretory status. For example, a tumor can obstruct blood flow to the heart, resulting in fainting, shortness of breath and chest pain, and heart failure [1, 2]. Functionally, paragangliomas produce an excess of catecholamines, which can cause a variety of symptoms, including hypertension, headache, supraventricular tachycardia, and anxiety [1, 2]. Heart failure can also develop due to the secretion of catecholamines by the tumor [1]. Paragangliomas usually manifest as a triad of hypertension, headache and palpitations [5].
In our case, taking into account the secretion of catecholamines, sick sinus syndrome, a high risk of bleeding, and tumor fragmentation, the first stage was to achieve size reduction of the tumor by means of embolization with coils of the afferent feeding the heart tumor. However, due to several sources of blood supply to the new-growth, this treatment method did not lead to the desired effect. In this regard, the tactics of open surgical intervention was chosen to remove the newgrowth with the reconstruction of heart chambers. According to the data of postoperative biopsy, removed tumor was paraganglioma. Positron emission computed tomography was performed, in which no remnants of a malignant formation were found, as well as metastases in other organs. In this regard, it was decided to refrain from chemotherapy, but the patient is registered at the oncological dispensary.
CONCLUSION
This experience shows the importance of a multidisciplinary and personalized approach in treatment of patients in a multidisciplinary hospital.
Список литературы A multidisciplinary approach to the treatment of malignant heart tumor
- Alakeel F., Al Sannaa G., Ibarra-Cortez S.H., Reardon M.J., Czerniak B., Chan E.Y., Ro J. Cardiac paragangliomas: A case series with clinic pathologic features and succinate dehydrogenase B immunostaining. Annals of Diagnostic Pathology, 2020, No. 45, р. 151477. DOI: 10.1016/j.anndiagpath.2020.151477
- Alam A., Dib E., Hall S., Gonzales G., Guerrero-Miranda C. Heart failure resulting from highly invasive primary cardiac paraganglioma. JACC, 2020, March, No. 24, Vol. 75, р. 11.
- Wcislak S.M., King W.S., Waller B.R., Goins N., Dickson P.V. Multifocal pheochromocytoma-paraganglioma in a 29-year-old woman with cyanotic congenital heart disease. Surgery, 2019, No. 16, 165(1), рр. 228-231. DOI: 10.1016/j.surg.2018.08.033
- Chang S.H., Yapar I., Kozower B.D. Aorticopulmonary paraganglioma with symptomatic postoperative bradycardia. The Annals of Thoracic Surgery, 2020, May, No. 109, Issue 5, рр. 367-369. DOI: 10.1016/j.athoracsur.2019.08.046
- Berona K., Joshi R., Woo Y.J., Shrager J. Postpartum diagnosis of cardiac paraganglioma: a case report. The Journal of Emergency Medicine, 2018, October, No. 55, Issue 4, рр. 101-105. DOI: 10.1016/j.jemermed.2018.05.034


