Analysis of CD3, CD68, CD163 and CK-19 expression in the thymuses of neonates with infectious diseases
Author: Dmitry A. Mudrak, Galina N. Maslyakova
Journal: Saratov Medical Journal @sarmj
Article in issue: 3 Vol.5, 2024.
Free access
Objective: to identify the expression patterns of immunohistochemical markers, CD3, CD68, CD163 and CK-19, in thymus cells of neonates with an enlarged thymus who died from infectious diseases. Materials and Methods. The study material was autopsy material of infants of the early and late neonatal periods (n=33) who died in medical hospitals of Saratov. The causes of death were pneumonia (n=17) and sepsis (n=16). The morphological material was divided into two groups: Group 1 (comparison group) included children whose thymus gland weight corresponded to the age norm (n=19); Group 2 (study group) comprised children whose thymus weight exceeded the age norm (n=14). The study assessed the expression of the following markers: CD3, CD68, CD163 and CK-19. Results. We established that with an increase in the thymus mass, the proportion of CD3+ cells in its cortex exhibited a 2.7-fold increase (p=0.009), the proportion of CD68+ cells demonstrated almost threefold increase (p=0.009), whereas the share of CD163+ cells diminished by 10% (p=0.005) and CK-19 positive cells did not form a network. Conclusion. An increase in the thymus mass in infants of the early neonatal period with infectious diseases is accompanied by disruption in the processes of lymphocyte migration and differentiation.
Thymus, infectious diseases, immunohistochemistry, CD3, CD68, CD163, CK-19
Short address: https://sciup.org/149147118
IDR: 149147118 | DOI: 10.15275/sarmj.2024.0302
Text of the scientific article Analysis of CD3, CD68, CD163 and CK-19 expression in the thymuses of neonates with infectious diseases
© This article is an open access publication. Russian Text. Published in Saratov Journal of Medical Scientific Research. 2024; 20 (3): 327–332. ISSN 1995-0039.
The thymus gland is the central organ of immunogenesis. Among its most important functions is antigen-independent differentiation of T cells. For the formation of an adequate cellular link of immunity, it is crucial that optimal conditions for the maturation of T cells migrating from the bone marrow to the cortex of the thymus are present.
Under the impact of infections, congenital disorders, and other factors, dysfunctions of the thymus are observed [1]. These disorders are of greatest importance in childhood, especially during infancy (from birth to 1 year of age), since at this time the child is more susceptible to the effect of unfavorable factors due to the functional imperfection of various organs and systems [2].
In addition to T lymphocytes, the thymus gland also contains B lymphocytes, plasma cells, eosinophils, neutrophils, histiocytes, and mast cells [3]. Among the lymphocyte populations, hematopoietic precursors of CD117+, CD3+, CD4+ and CD8+ T cells have been detected [4]. Correct differentiation of thymus lymphocytes directly depends on the microenvironment of T cells in the thymus gland. Macrophages present antigen to T lymphocytes. With adequate interaction between the antigen-presenting cell and the lymphocyte, an antigen-dependent immune reaction begins [5]. There is evidence in the literature that an increase in the thymus is a risk factor for the development of
complications in children with infectious diseases [6]. However, at present, there is no consensus on the assessment of this symptom.
These days, the issue of thymus morphology in conditions of its increased mass and various diseases remains insufficiently studied.
The goal of our study was to identify the features of expression of immunohistochemical (IHC) markers, CD3, CD68, CD163 and cytokeratin-19 (CK-19), in thymus cells of neonates with an enlarged thymus who died from infectious diseases.
Materials and Methods. The study material was autopsy material of neonates (n=33) who died in Saratov hospitals. The causes of death were pneumonia (n=17) and sepsis (n=16). The morphological material was divided among two groups: Group 1 (comparison group) with neonates whose thymus mass corresponded to the age norm (n=19) and Group 2 (study group) including neonates whose thymus mass exceeded the age norm (n=14). Excess thymus mass (i.e., above the age norm) was assessed using centile tables of thymus index values [6].
The collected samples were fixed in 10% formalin solution, after which we performed standard histological processing and embedding in paraffin. Then, sections with a thickness of 4-5 μm were prepared using a rotary microtome. The obtained sections were subjected to IHC reaction and hematoxylin staining. Morphometric analysis was performed using a LOMO-103 microvisor.
For the IHC reaction, we used rabbit antibodies (AB) to CD3 (monoclonal, dilution 1:1000, Abcam, UK), CD68 (polyclonal, dilution 1:100, Spring Bioscience, USA), CD163 (polyclonal, dilution 1:200, Spring Bioscience, USA), CK-19 (monoclonal, dilution 1:50, DAKO, USA). Staining was performed using the Reveal–Biotin-Free Polyvalent DAB multimer detection system (Spring Bioscience Corp., USA). To assess the specificity of immunostaining, a negative control was used in each case (sections were treated with control AB instead of primary AB), which resulted in the absence of specific immunostaining.
The reaction with AB to CD3 was performed to assess the activity of thymopoiesis and to identify the population of mature T lymphocytes. The reaction with AB to CD68 was performed to identify macrophages, monocytes, basophils, mast cells and B cells. AB to CD163 was used to isolate macrophages and monocytes from this group. CK-19 was employed to identify thymic epithelial cells.
The expression level was assessed by calculating the percentage of cells with positive marker expression out of 1000 cells in 10 random fields of view at a magnification of ×774.0. The assessment was performed separately in the thymus cortex and medulla.
Statistical data processing was performed using the Microsoft Excel 2010 software. Data distribution analysis was performed using the Shapiro-Wilk test. The distribution was different from normal. Based on this, the statistical significance of the obtained differences was assessed using the nonparametric Mann-Whitney U test. The following parameters were calculated to describe the groups: median (Me), 25th and 75th percentiles (Q25-Q75), minimum value (min) and maximum value (max).
The study was approved by the Ethics Committee of Saratov State Medical University (protocol #6 of 06 February 2018.
Results. General microscopy revealed the pronounced edema and the thymus capsule full of blood, along with some increase in the number of lobules in the enlarged thymus. In most cases, differentiation of the medulla and cortex was preserved in Group 1. In Group 2, an increase in the cortex was noted, while it was impossible to distinguish the medulla and the cortex in some lobules. Hassall’s corpuscles in the thymus of Group 1 children exhibited a conventional structure and were located mainly in the medulla of the lobe. In Group 2, a variable location of Hassall’s corpuscles was noted over the entire area of the lobe. Besides that, we revealed signs of their degradation – viz., thymic bodies deformed by cysts prevailed.
It was established that the total number of cells in the field of view in the group with an increased thymus mass was 28.3% higher in the cortex (p<0.001). The total number of cells in the medulla of the thymus did not differ statistically significantly between groups.
The IHC study showed that in the group of children with an enlarged thymus, the expression of the CD3 marker in the cortex exceeded the corresponding parameter in the thymus of Group 1 children. No significant differences in the number of these cells in the medulla of the thymus were detected ( Table, Figure 1 ).
Table. Expression of immunohistochemical markers (%) in the cortex and medulla of the thymus
|
Localization in the thymus |
Marker |
Group, Me [ Q 25 - Q 75 ]; (minmax) |
р |
|
|
1 |
2 |
|||
|
Cortex |
CD3 |
14.2 [9.5 23.1]; (6.8 50.0) |
37.7 [36.8 41.1]; (21.1 48.4) |
0.009 |
|
CD68 |
4.1 [3.7-5.6]; (3.6-6.9) |
13.8 [7.3 14.3]; (3.8 21.7) |
0.001 |
|
|
CD163 |
25.9 [21.3 33.3]; (16.7 49.5) |
15.5 [11.3 25.0]; (6.4 30.0) |
0.005 |
|
|
Number of cells |
145 [125 167]; (114 187) |
186 [170 225]; (137 253) |
<0.001 |
|
|
Medulla |
CD3 |
59.9 [37.4 65.1]; (29.2 76.2) |
57.7 [48.6 64.9]; (37.7 68.7) |
0.761 |
|
CD68 |
0 [0-2.1]; (0 3.1) |
1.52 [0-3.9]; (0-6.9) |
0.178 |
|
|
CD163 |
16.7 [14.4 25.5]; (8.5 35.2) |
12.6 [12.4 13.9]; (8.4 15.8) |
0.008 |
|
|
Number of cells |
120 [117 154]; (101 179) |
150 [129 167]; (121 198) |
0.286 |
|
We used the nonparametric Mann-Whitney test; differences were considered significant at p <0.05.
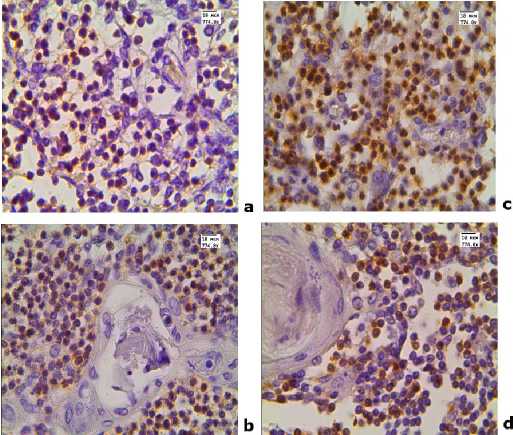
Figure 1. CD3 expression in the thymus of children who died from infectious diseases. Immunohistochemical reaction. Magnification X774.0. Here and below, in
Figures 2-4, groups of children are represented as follows:
a, b - Group 1 (with normal thymus mass); c, d - Group 2 (with increased thymus mass).
a, c - cortex; b, d - medulla.

Analysis of CD3, CD68, CD163 and CK-19 expression in the thymuses of neonates with infectious diseases
The number of cells with positive expression of the IHC marker, CD68, exhibited a similar trend: it was higher in the cortex of the thymus in children with an enlarged thymus, while no statistically significant differences in the level of expression in the medulla of the organ were revealed ( Table, Figure 2 ).
The expression of the CD163 marker in the thymus sections of Group 2 subjects significantly decreased in both the cortex and the medulla ( Table, Figure 3 ).
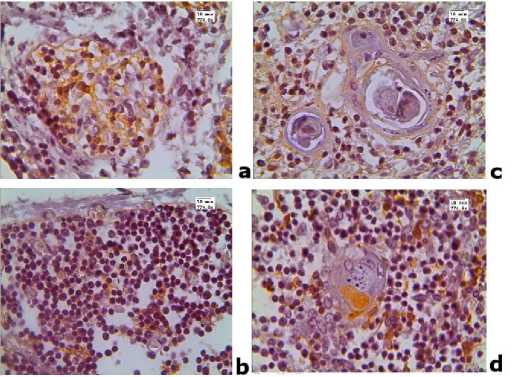
In the group of children with enlarged thymus mass, cytokeratin-19-positive cells were not distributed evenly: they were located mainly in the cortex directly at the interlobular septa (Figure 4b) and did not form a network in either the cortex or the medulla (Figure 4). The proportion of CK-19 positive cells in the medulla did not change significantly and was approximately 8%. Hassall’s corpuscles included cells of epithelial origin with positive expression of this marker. The proportion of thymic bodies with positive expression of CK-19 in both groups was approximately 70% ( Figure 4d ).
VA ■ .
Figure 4. Expression of cytokeratin-19
■ . »’СЯЬ
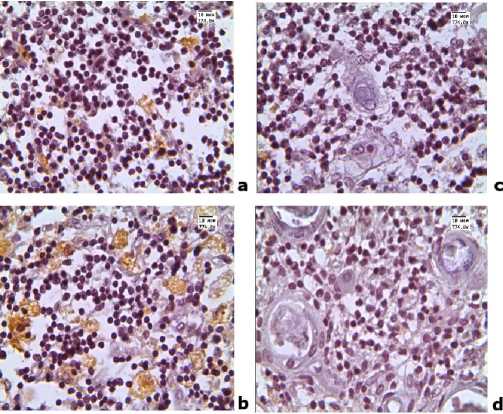
Figure 2. CD3 expression in the thymus of children who died from infectious diseases
d
Figure 3. Expression of CD163 in the thymus of children who died from infectious diseases
Discussion
It is well known that a significant proportion of cortical thymic cells are precursor cells migrating from the bone marrow. Further differentiation processes of these cells occur in the cortex of the thymus. Mature lymphocytes migrate to the medulla, from where they enter the bloodstream [7].
Our study confirmed that the increase in thymus mass occurs due to an enlargement of its cortex. We discovered that in neonates with an increased thymus mass, 2.7 times more CD3+ thymocytes were detected in the cortex. It is noteworthy that statistically significant differences in the expression of this marker in the thymus medulla were not observed. Therefore, with an increase in thymus mass, T cells accumulate in the cortex of the thymus.
Normally, the blood–thymus barrier of epithelial reticular cells is formed at the border between the cortex and medulla. Hence, this barrier isolates the medulla. Based on this, an increase in the number of CD3+ cells in the cortex may be a manifestation of a barrier dysfunction, which may lead to a prolonged stay of thymocytes in the cortex. This fact implies a disruption of thymocyte migration. However, this issue requires further study, since an increase in the number of cortical cells may be associated with increased migration of progenitor cells from the bone marrow; some authors consider CD3 as a marker of thymopoiesis activation [2]. Other researchers note that CD3 expression cannot be interpreted unambiguously, because both mature and immature T lymphocytes can exhibit positive staining [8].
It should be noted that the number of CD3+ cells in the medulla of the thymus, where the final stage of lymphocyte differentiation occurs, did not differ between groups. Therefore, an increase in the mass of the thymus gland was not a sign of cellular immunity activation, since these cells cannot enter the bloodstream from the cortex of the thymus to perform their functions properly [4].
Many researchers used CD68 to identify macrophages in the thymus [9-11]. Meanwhile, other studies showed that CD163 is a more specific marker of macrophages. The results of our study revealed multidirectional dynamics of changes: CD68 expression increased exclusively in the cortex of the thymus in neonates with an enlarged thymus, while CD163 expression diminished in both the cortex and medulla of the thymus in the same group of neonates. Consequently, an increase in CD68 expression may be due to an increase in the number of basophils, mast cells, and B cells.
A number of authors note the important role of macrophages in the differentiation of T cells. It is macrophages that participate in the negative selection of damaged lymphocytes. A reduction in the expression level of CD163 in the thymus of neonates in Group 2 indicates a decrease in the level of negative selection, which means that it leads to an increase in the number of defective lymphocytes.
Mast cells have the ability to reduce the suppressor activity of regulatory T cells, which also include thymus macrophages, by releasing histamine. Thus, under conditions of the thymus enlargement, in addition to a decrease in the number of macrophages, there is an elevated suppression of their function. This issue also adversely affects the processes of negative selection of thymocytes, i.e., it disrupts their normal differentiation.
CD68 is not a specific marker of macrophages and mast cells; in addition to these cells, B cells also exhibit a positive reaction. Some authors believe that B cells can participate in the process of negative selection [12]. Hence, it would be possible to explain the compensation of negative selection by an increase in the number of B cells. However, other authors do not consider the theory of B cell involvement in the processes of defective thymocyte elimination to be sufficiently substantiated [13]. Therefore, this issue requires further study.
There is information in the literature that Hassall’s corpuscles are the final stage of thymic epithelial cell differentiation [14]. In the group with normal thymus mass, CK-19 positive cells form a network both in the cortex and in the medulla of the thymus. Probably, this network serves as a place of communication between lymphocytes and epithelial cells, which provides optimal conditions for T cell differentiation. Hence, the disruption of this network in the thymus, which we observed in the group of neonates with an enlarged thymus, is another sign of morphofunctional insufficiency of the thymus with an enlarged mass.
Conclusion
Analysis of the expression of CD3, CD68, CD163 and CK-19 markers in sections of the thymus in children who died from infectious diseases demonstrated that an increase in thymus mass in them implies a disruption in the processes of migration and differentiation of lymphocytes, which may indicate a functioning disorder in the cellular component of immunity.
Informed consent for publication: The authors obtained written consent from the patients’ legal representatives for the analysis and publication of medical data.
Author contributions : All authors contributed equally to the preparation of the manuscript.
Conflict of interest: None declared by the authors.
References Analysis of CD3, CD68, CD163 and CK-19 expression in the thymuses of neonates with infectious diseases
- Loginova NP, Chetvertnykh VA, Chemurziyeva NV. Morphofunctional changes of thymus tissues in children with congenital heart defects. Morphology 2016; 149 (1): 57-63. (In Russ.) https://pubmed.ncbi.nlm.nih.gov/27487665
- Lavini CA, Moran U, Morandi R. Thymus Gland Pathology. Clinical, Diagnostic, and Therapeutic Features. Milan: Springer-Verlag Italia 2008; 273 p.
- Matveev VA. Method of thymomegaly detection in young children to predict the course of infectious processes: Instruction for use No. 047-0511. Minsk: Ministry of Health of the Republic of Belarus 2011; 6 p. (In Russ.)
- Pearse G. Normal structure, function and histology of the thymus. Toxicologic Pathology 2006; 34 (5): 504-14. https://www.doi.org/10.1080/01926230600865549
- Krivolapov YA, Leenman EE. Morphological Diagnosis of Lymphomas. Saint Petersburg: KOSTA 2006; 208 p. (In Russ.)
- Taylor PR, Martinez-Pomares L, Stacey M, et al. Macrophage receptors and immune recognition. Annu Rev Immunol. 2005; 23: 901-44. https://www.doi.org/10.1146/annurev.immunol.23.021704.115816
- Bruun JM, Helge JW, Richelsen B, Stallknecht B. Diet and exercise reduce low-grade inflammation and macrophage infiltration in adipose tissue but not in skeletal muscle in severely obese subjects. Am J Physiol Endocrinol Metab. 2006; 290: 961-7. https://www.doi.org/10.1152/ajpendo.00506.2005
- Mäkitie T, Summanen P, Tarkkanen A, Kivelä T. Tumor-infiltrating macrophages (CD68(+) cells) and prognosis in malignant uveal melanoma. Invest Ophthalmol Vis Sci. 2001; 42: 1414-21. https://pubmed.ncbi.nlm.nih.gov/11381040
- Ferrero I, Anjuere F, Martin P, et al. Functional and phenotypic analysis of thymic B cells: Role in the induction of T cell negative selection. Eur J Immunol. 1999; 29 (5): 1598-609. https://www.doi.org/10.1002/(SICI)1521-4141(199905)29:05<1598::AID-IMMU1598-3.0.CO;2-O
- Starskaya IS, Polevshchikov AV. Morphological features of thymus atrophy under stress. Immunology 2013; 5: 271-7. (In Russ.).
- Yastrebova SA, Illarionova SV, Zaitseva NA, Sergeeva VE. Reaction of CD68 positive cells of spleen and thymus to the introduction of immunomodulators. Responses of CD68 positive cells in the spleen and thymus to the introduction of immunomodulators. International Journal of Applied and Fundamental Research 2016; 4-3: 589-93. (In Russ.)
- Bearman RM, Bensch KG, Levine GD. The normal human thymic vasculature: An ultrastructural study. Anat Rec. 1975; 183 (4): 485-97. https://www.doi.org/10.1002/ar.1091830402
- Mori K, Itoi M, Tsukamoto N. The perivascular space as a path of hematopoietic progenitor cells and mature T cells between the blood circulation and the thymic parenchyma. Int Immunol. 2007; 19 (6): 745-53. https://www.doi.org/10.1093/intimm/dxm041
- Postovalova EA, Makarova OV, Kosyreva AM, Mikhailova LP. Morphology of the thymus and features of its cellular composition in experimental acute and chronic ulcerative colitis. Archives of Pathology 2019; 81 (5): 53-63. (In Russ.) https://www.doi.org/10.17116/patol20198105153


