Comparison of hemodynamic changes and their management following subarachnoid block between normotensive and preeclamptic women undergoing cesarean section
Author: Chigurupalli K., Madabhattula G., Srivastava S., Purohit R., Rani U., Yadav B.B., Kalidindi D., Kintali S.S., Gehlot G.
Journal: Juvenis scientia @jscientia
Section: Оригинальные исследования
Article in issue: 6 т.9, 2023.
Free access
Introduction. Spinal anesthesia (SA) is widely used for cesarean sections, yet its safety in preeclamptic patients remains uncertain. This study explores the use of subarachnoid block (SAB) in preeclamptic parturients during cesarean sections. Patients and Methods. This study was a single-center hospital-based controlled clinical trial. 30 normotensive and 30 preeclamptic women undergoing cesarean section were included in the study. Heart rate, systolic blood pressure (SBP), diastolic blood pressure (DBP), mean arterial blood pressure (MAP) and SpO2 were evaluated at one, three, five, seven, nine, 11, 13, 15, 20, 25, 30, 40, 45, 50, 55 and 60 minutes intervals after giving the block. The independent samples t-test was used for statistical analysis.
Spinal anesthesia, pregnancy-induced hypertension, subarachnoid block, mephentermine
Short address: https://sciup.org/14129342
IDR: 14129342 | DOI: 10.32415/jscientia_2023_9_6_42-52
Сравнение гемодинамических изменений и потребности в их коррекции при проведении спинальной анестезии женщинам с нормальным артериальным давлением и пациенткам с преэклампсией во время кесарева сечения
Введение. Спинальная анестезия (СА) широко используется при кесаревом сечении, однако её безопасность у пациенток с преэклампсией (ПЭ) остаётся недостаточно изученной. В данном исследовании проведена оценка использования субарахноидальной блокады (САБ) у рожениц с преэклампсией во время кесарева сечения. Пациенты и методы. В одноцентровое контролируемое клиническое исследование включено 30 беременных женщин с нормальным артериальным давлением и 30 женщин с ПЭ, которым проводилось кесарево сечение. Частоту сердечных сокращений (ЧСС), систолическое артериальное давление (САД), диастолическое артериальное давление (ДАД), среднее артериальное давление (СрАД) и SpO2 оценивали через 1, 3, 5, 7, 9, 11, 13, 15, 20, 25, 30, 40, 45, 50, 55 и 60 минут после начала САБ. Для статистического анализа использовался t-критерий для независимых выборок.
Text of the scientific article Comparison of hemodynamic changes and their management following subarachnoid block between normotensive and preeclamptic women undergoing cesarean section
Spinal anesthesia (SA) or subarachnoid block (SAB) is a form of regional anesthesia and a kind of neuraxi-al block involving injection of opiods, local anesthetics or other permissive drug into the subarachnoid space. Spinal anesthesia offers many advantages for operation although the extent of its benefit is not agreed universally. It has a very rapid onset and provides a dense neural block which can produce highly effective pain relief for a wide variety of indications and may decrease patient morbidity after major surgery, moreover, failures are very infrequent [1, 2].
Advantages of spinal anesthesia include: easy technique, rapid onset, simple performance, requirement of minimum equipments and monitors, little effects on blood biochemistry, optimum levels of arterial blood gases, conscious patients during surgery and maintenance of airway patency, less postoperative care and optimum anesthesia [3].
Pregnancy-induced hypertension (PIH) constitutes major cause of morbidity and mortality in developing countries, and it accompanies 5–10% of all pregnancies [4, 5].
It is postulated that there is a functional imbalance between the endogenous vasodilators (prostacyclin, PG I2) and vasoconstrictors (thromboxane A2) leading to arteriolar vasospasm. There is intense vasoconstriction leading to hypoperfusion of vital organs. The hemodynamic profile is thus altered. Various cardiovascular (CVS) effects like labile blood pressure (BP), decreased colloid oncotic pressure, intravascular volume depletion, increased systemic vascular resistance, hypertension, and hypercoagulable states can coexist. The deleterious effects on central nervous system include cortical blindness, cerebral edema, seizures and cerebrovascular accidents. Renal system involvement can manifest as proteinuria, decrease in renal blood flow with decreased glomerular filtration rate, increased blood urea nitrogen and creatinine. Elevated liver enzymes and decreased plasma serum cholinesterase levels reflect liver involvement. Airway edema, pulmonary edema, and ventilation perfusion mismatch may be associated as a result of respiratory system involvement. Fetal compromise results as a consequence of uteroplacental insufficiency, placental abruption, chronic fetal hypoxia, intrauterine growth retardation (IUGR), and premature labor and delivery. The definitive cure of PIH is the delivery of fetus and placenta. Termination of pregnancy may be required in the form of induction of labor or cesarean section (CS), which may be a planned or an emergent procedure. Anesthesiologist comes into the picture when cesarean delivery is contemplated. CS may be indicated either in maternal or in fetal interest. The maternal indications may be uncontrolled BP, unfavorable cervix, failed induction of labor, or antepartum hemorrhage [9].
However, anesthesia for cesarean section in a patient with preeclampsia is far more complicated than in an otherwise normal pregnancy for several reasons. Apart from the risks of high incidence of intrauterine growth restriction, fetal distress and prematurity, there are risk of increased perioperative morbidity due to altered hemodynamics in these patients [7– 11]. Either of the two techniques — general anesthesia (GA) or central neuraxial blockade (CNB) — may be employed for anesthesia [6]. Regional anesthesia is often considered to be a safer option in obstetric cases, as the hazards of difficult airway associated with weight gain and edema can be avoided. The technique of anesthesia has to be chosen judiciously based on individual patient condition [6].
Spinal anesthesia seems to be well-suited for in patients undergoing cesarean section because of the short interval from injection to surgical anesthesia [12].
However, spinal anesthesia has not yet been popular due to the common belief that the sudden and extensive sympathetic blockade following subarachnoid block (SAB) will result in severe hypotension that will endanger maternal and fetal safety. Recently, some studies challenged this view and suggested that SAB may in fact be an appropriate choice in preeclamptic women [13, 14].
The ideal technique for anesthesia has been a long controversy among the obstetric anesthesiologists as the risk of hypotension and altered hemodynamics has influenced the choice of anesthesia [7].
The analysis of anesthesia-related deaths during obstetric delivery in the United States from 1979–1990 indicated that general anesthesia is related to 16.7 times increased mortality risk compared with neurax-ial blockade for cesarean delivery [15].
Advances in anesthesia drugs and techniques reduced that figure to 1.7 times in between 1979 and 2002, [16] but still more favourable outcomes are found with neuraxial anesthesia. Less morbidity and mortality, less failure, dense anesthesia, easy technique, provision of adequate operating conditions in a shorter time and several other advantages have placed neuraxial anesthesia, particularly, subarachnoid block, as a more preferable mode of anesthesia for elective cesarean section to epidural block or general anesthesia [7].
Recently, some studies have challenged this view and suggested that SAB may in fact be an appropriate choice in preeclamptic women. Yet, this evidence is based on the very few published information regarding the use of SAB in preeclamptic patients [13, 14]. This prompted us to validate the safety of SAB in pre-eclamptic parturients undergoing LSCS.
AIMS AND OBJECTIVES
Aim. This study was aimed to evaluate the hemodynamic changes, their management and fetal outcomes following spinal anesthesia between normotensive and severe preeclamptic pregnant women undergoing cesarean section.
Objectives:
The objectives of this study were:
-
1. To compare the hemodynamic changes following subarachnoid block between normotensive and severe preclamptic women undergoing cesarean section.
-
2. To assess the dosage of mephentermine required to maintain the hemodynamic stability after subarachnoid block in cesarean section.
METHODOLOGY
The present study was conducted in the Department of Anesthesiology, King George Medical College and Hospital, Visakapatnam, India.
Study design. This study was a single-center hospital-based controlled clinical trial.
Study Period. The present study was conducted during the period from January 2021 to October 2022.
Source of Data. Normotensive pregnant women and pregnant women with severe preeclampsia posted for cesarean section under spinal anesthe- sia under the Department of Anesthesiology, King George Medical College and Hospital, Visakapatnam, Andhra Pradesh were enrolled.
Sample size and sampling procedure. A total of 60 pregnant women that is 30 normotensive and 30 severe preeclamptic women were studied.
The sample size was determined using a desired power of 0.8 and an error of 0.05. Hence, Zα was 0.1 i.e. 1.96, Zβ was 0.3 i.e. 0.84. The sample size was determined using the following formula.
Where,
2 ( Z a +Z e ) 2x ( SD i +SD 2 ) ( X 1 -X 2 ) 2
Zα = 1.965 for α =0.05
Zβ = 0.84 for β =0.3
SD1 = 2.77^3 (Standard deviat i on for fall in SBP after SAB based on recent study by Mitra M. et al. [7] (2016);
SD2 = 1.28≈1(Standard deviation for fall in SBP after SAB based on recent study by Mitra M. et al. [7] (2016);
X1 = 10.39-10 (Mean fall in SBP after SAB based on recent study by Mitra M. et al. [7] (2016);
X2 = 5.01≈5 (Mean fall in SBP after SAB based on recent study by Mitra M. et al. [7] (2016).
Hence
2 ( 1.96+0.84 ) 'Ч32+Г ) n= ( 10-5 ) 2
Therefore, n = 16.50 ≈ 17
the minimum effect size to estimate the effect of SAB on hemodyanamic profile was 17 in each group. However, in order to have uniformity in results and as 60 women were eligible and consented to participate in the study a total sample size of 60 patients divided into two groups of 30 each was considered.
The selected women were divided into two groups of 30 each as below.
Group N: 30 normotensive pregnant women undergoing LSCS.
Group PE: 30 severe preeclamptic pregnant women undergoing LSCS.
Selection Criteria
Inclusion criteria
— Normotensive or severe preclamptic pregnant women undergoing elective LSCS under spinal anesthesia with ASA Grade I or II
-
— Women aged between 18 to 30 years and weight 45 to 80 Kg
-
— Women with singleton pregnancy
Exclusion criteria
-
— Pregnant women with eclampsia
-
— Pregnant women with contraindications to subarachnoid block, having local site infection, septicaemia, raised intracranial pressure (ICT)
-
— Elderly women and obesity (body mass index [BMI] >35 kg/m2)
-
— Multiple pregnancy
-
— Pregnant women with cardiac disease, renal disease, diabetes mellitus, coagulopathy and those who refused subarachnoid block
-
— Pregnant women with placenta praevia, abruptio placenta
Ethical clearance
The study was approved and ethical clearance was obtained from Institutional Ethics Committee, King George Medical College, Visakhapatnam, Andhra Pradesh.
Pre-anesthetic evaluation
A thorough pre-anesthetic evaluation was performed by taking history. In all the patients, height, weight, basal heart rate, respiratory rate and blood pressure were measured and recorded. All parturients were premedicated with oral ranitidine (150 mg) 2 h prior to the surgery. In addition, in severe pre-ec-lamptic parturients, antihypertensive medication was continued. After establishing IV access with 18 G cannula prehydration was done with 10 ml/kg body weight of lactated ringer (RL) solution. The volume of administered fluid was not restricted in the severe preeclamptic patients because of the contracted intravascular volume in this group of patients and the high incidence of hypotension caused by spinal anesthesia-induced sympathetic blockade. Standard multichannel monitor was attached and baseline hemodynamic values of various parameters (HR, SBP, DBP, MAP) were recorded. Baseline BP was measured as the mean of the three readings taken 5 min after arrival in the operation theatre and before doing any invasive procedures.
Anesthesia procedure
All the blocks were perfomed by experienced anesthesiologists. After proper asepsis and draping with betadine, SAB was administered with 25 G spinal needle at L4–5 interspace in sitting posture with 10 mg hyperbaric 0.5% bupivacaine. Infusion of RL was continued at the rate of 5 ml/kg/h. The height of the sensory block was assessed using a pinprick test, and a 10°-15° head down-tilt (Trendelenburg position) was initiated if a T6 sensory level was not achieved at 10 minutes after the spinal injection. Surgery was allowed as soon as upper level of sensory block reached T6. SBP, DBP, MAP, and HR were recorded every 2 min for 15 min and every 5 min thereafter until completion of surgery. Hypotension (defined as MAP < 30% of the baseline) was treated with 6 mg mephentermine IV bolus and the dose was repeated at a 5 min interval if required to maintain MAP within 30% of baseline. Bradycardia (HR < 60 beats/min) if associated with hypotension was treated with 0.6 mg IV atropine (maximum 1.8 mg).
In cases of failed anesthesia or inadequate anesthesia even after 15 minutes general anesthesia was given. No sedation was given to any patients intraoperatively. Oxygen (5 L/min) by facemask was given until delivery of the baby. Fluid therapy was maintained with lactate ringer solution (10 ml/kg/hr).
Outcome variables
Sensory level block
Sensory level was assessed bilaterally with the use of temperature (by cold water swab) and by pin prick at the midclavicular line while motor block was assessed by using Bromage score [17].
-
— 1 = unable to move feet or knees.
-
— 2 = able to move feet only.
-
— 3 = just able to move knees.
-
— 4 = full flexion of knee and feet
Hemodynamic monitoring
Heart rate, SBP, DBP, MAP and SpO2 were evaluated at one, three, five, seven, nine, 11, 13, 15, 20, 25, 30, 40, 45, 50, 55 and 60 minutes intervals after giving the block.
Total dose of mephentermine
The total dosage of mephentermine consumed after subarachnoid block was noted.
Statistical Analysis
Data obtained was coded and entered into Microsoft excel spreadsheet. The data was analysed by SPSS statistical software version 20.0. The categorical data was expressed in terms of rates, ratios and percentage and continuous data was expressed as mean ± standard deviation (SD). Chi square test and Fisher’s exact test were used to compare the categorical data and continuous data was compared with independent sample t test. A probability value (p value) of less than or equal to 0.05 at 95% confidence interval was considered as statistically significant.
RESULTS
In the present study 66.7% of the women were aged between 26 to 30 years in group N and group PE (p=1.000). Age distribution is presented in Figure 1.
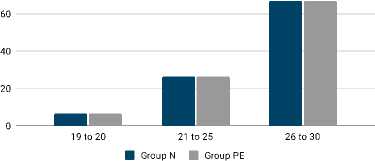
Figure 1. Comparison of age distribution
It was observed that the mean age, height, and pulse rate were statistically similar in both the groups (Figure 2). Meanwhile, the weight, SBP, DBP and MAP were significantly higher in group PE (p<0.050).
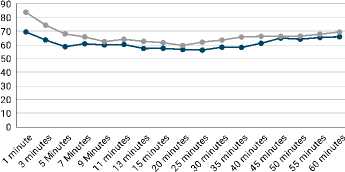
The comparison of the mean heart rate at different intervals is as shown in Figure 3. It was observed that the mean heart rate was comparable in both the groups at all the intervals (p>0.050).
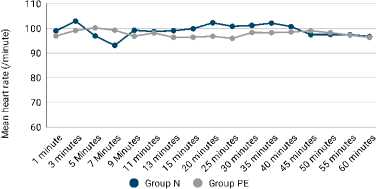
Figure 3. Comparsion of heart rate after surgery
The comparison of mean SBP at different intervals is as shown in Figure 4. It was observed that the mean SBP was significantly lower in group N at one minute, three, five, 25, 35, 40, 45, 50, 55 and 60 minutes intervals (p<0.050).
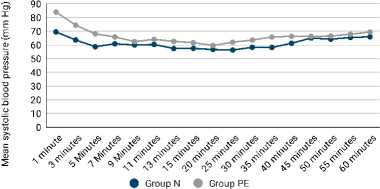
Figure 4. Comparsion of systolic blood pressure after surgery
The comparison of mean DBP at different intervals is as shown in Figure 5. It was observed that the mean DBP was significantly lower in group N at one minute, three, five, and 35 minutes intervals (p<0.050).
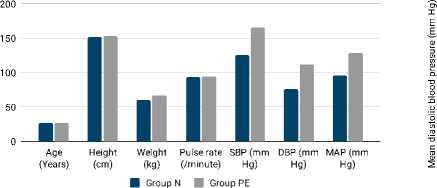
Figure 2. Comparison of baseline characteristics
• Group N ® Group PE
Figure 5. Comparsion of diastolic blood pressure after surgery
The comparison of mean MAP at different intervals is as shown in Figure 6. It was observed that the mean MAP was significantly lower in group N at one minute, three, five, 25, 35 and 60 minutes intervals (p<0.050).
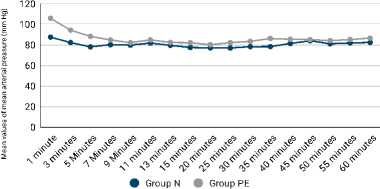
Figure 6. Comparison of mean arterial pressure after surgery
The comparison of oxygen saturation at different intervals is as shown in Figure 7. It was observed that the mean oxygen saturation was comparable in both the groups at all the intervals (p>0.050).
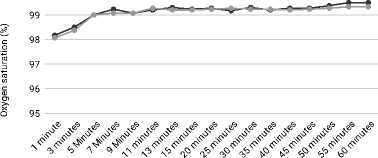
• Group N • Group PE
Figure 7. Comparsion of oxygen saturation after surgery
In this study, the consumption of mephenter-mine (Figure 8) was significantly higher in group N (7.10±5.13 mg) compared to group PE (2.00±3.96 mg) (p<0.001).
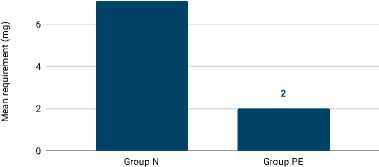
Figure 8. Comparison of mephentermine requirements
Adverse fetal outcomes were not observed in both studied groups.
DISCUSSION
In the present study, despite of alteration in SBP, DBP and MAP, the mean oxygen saturation was comparable in both the groups at all the intervals (p>0.050). The observed blood pressure values over a continuum does not truly reflect the hemodynamic alteration attributed to physiological changes imparted by SAB in both the groups. The blood pressure values reflect the combined outcome of the physiological effects, ongoing medications and anesthesia management strategy and should be interpreted accordingly [7].
In this study, although significant differences were noted with regard to SBP, DBP and MAP, the mean consumption of mephenterine was significantly higher in normotensive women (7.10±5.13 mg) compared to women with severe preeclampsia (2.00±3.96 mg) (p<0.001). After establishing SAB, blood pressure decreased in both the groups from the baseline, but the minimum SBP, DBP, and MAP recorded during the observation period were always higher in the severe preeclamptic group. The lowest SBP noted among normotensive women was 106.67±15.01 at five minutes interval which gradually increased to 114.37±9.99 mm Hg at 11 minutes interval, gradually decreased to 109.03±10.48 mm Hg at 20 minutes interval and 109.40±10.48 mm Hg at 25 minutes interval. Meanwhile, in women with severe preeclampsia the lowest SBP was noted at 20 minutes interval (113.07±16.05 mm Hg) and at nine minutes interval (113.37±13.23 mm Hg). Similarly, the lowest DBP noted among normotensive women was 57.37±9.63 mm Hg at 13 minutes interval while in women with severe preeclampsia the lowest DBP was noted as 59.57±13.33 mm Hg at 20 minutes interval. The lowest SBP, DBP, and significantly lower SBP, DBP and MAP values among normotensive women as discussed above at various intervals resulted in higher vasopressor requirements to treat the episodes of hypotension. These observations suggest that SAB in normotensive women results in hypotension. These observations are similar to a study by Saha D. et al. (2013) who compared the hemodynamic effect and vasopressor requirement after SAB between normotensive parturients and severe preeclamptic women undergoing cesarean section [5]. After establishing SAB, blood pressure decreased in both the groups from the baseline, but the minimum SBP, DBP, and MAP recorded during the observation period were always higher in the severe preeclamptic group (118.8 ± 6.36, 71.2 ± 12.16, 74.2 ± 7.34, respectively) in comparison with normotensive group (91.9 ± 16.9, 48.76 ± 12.72, 53.7 ± 6.36, respectively), with statistically significant difference (P < 0.0001). Severe preeclamptic patients needed significantly less phenylephrine to treat hypotension (151.1±70 µg in normotensive and 48.3±35.35 µg in severe preeclamptic women), and the difference was statistically significant (p<0.0001). These findings are strong in agreement with the present study.
The present study also corroborates with another study results by Aya et al. (2003), comparing the incidence and severity of hypotension and ephedrine consumption in 30 preeclamptic women and 30 healthy parturients [18]. They found that SAB-induced hypotension was 6 times less prevalent in preeclamptic women and they required significantly less ephedrine to treat it.
In a study by Dyer et al. (2008) the authors observed the hemodynamic responses to SAB for cesarean delivery in 15 severe preeclamptic parturients and used the beat-to-beat monitoring of cardiac output (CO) for this purpose [19]. The effect to phenylephrine on CO was also observed. They concluded that the changes in CO after SAB in severe preeclamptic women were insignificant, and the reduction in MAP was easily restored by phenylephrine without any decrease in maternal CO.
The findings of the present study are also comparable with a recent study by Mitra M. et al. (2016) where the authors have found significant differences in SBP, DBP and MAP at different points of times in both the groups [7]. One probable explanation of this may be the use of invasive arterial blood pressure monitoring in place of noninvasive monitoring unlike other studies. Also the preoperative blood pressure values were significantly different in both the groups. More phenylephrine consumption was noted in the normotensive group. This indicated higher incidence of hypotension in the normotensive group and also contributed to the dissimilar magnitude of changes in blood pressure at different points of times. The authors also emphasized on the latter fact as most studies compared different blood pressure values over a point of time with a significant difference in baseline blood pressure values and significant difference in mean vasopressor consumption.
In a normal pregnancy, increased synthesis of endogenous vasodilators like prostaglandins (PGs) and nitric oxide (NO) produces a vasodilated state, and there appears an increased dependence on sympathetic vasoconstriction for control of vascular tone. This explains the sudden and excessive hypotension after sympathetic blockade produced by SAB in them [20]. In preeclampsia, vascular endothelial damage occurs, which produces increased amount of endogenous vasopressors like thromboxane and endothelin that are responsible for maintaining vessel tone. Sympathetic block following SAB does not alter this vascular response, limiting the excessive fall of BP in preeclamptic patients [15, 18].
Visalyaputra et al. (2005) conducted a multicenter randomized study to compare the hemodynamic effects of spinal and epidural anesthesia for cesarean delivery in severely preeclamptic patients and observed in spite of the hypotension (SBP < or + 100 mmHg) being more frequent in the spinal group than the epidural group (51% versus 23%), the duration was short and it was easily treatable with ephedrine [21]. Overall, the present study showed that, despite the significant differences in hemodynamic profiles, especially higher SBP, DBP and MAP, hypotension following spinal anesthesia administered for cesarean section was significantly less common in severe preeclamptic women than in normotensive women as mephentermine requirements were significantly lower in severe preeclamptic parturients. Hence, subarachnoid block in severe preeclamptic patients offers better perioperative hemodynamic stability, less hypotension, less vasopressor consumption and comparable neonatal outcomes. However, these observations require further validation due to potential limitations of this study viz. a single-center study involving a relatively small sample and other associated maternal complications were not consid- ered. Hence, further multicenter studies involving larger samples and considering other maternal complications may show the pertinent usefulness of SAB in women with severe preeclampsia.
CONCLUSION
Based on the findings of this study, it may be concluded that there are significant differences in hemodynamic profiles, in particular higher SBP, DBP and MAP, in women with severe preeclampsia compared to normotensive women undergoing cesarean section following subarachnoid block. However, SAB does not alter heart rate and oxygen saturation. At the same time, hypotension following spinal anesthesia ad- ministered for cesarean section was significantly less common in severe preeclamptic women than in normotensive women as vasopresser requirements were significantly lower in severe preeclamptic parturients.
Funding: The authors declare no funding.
Conflict of interest: The authors declare no conflict of interest.
Author contributions: All authors confirm the authorship according to the international criteria of ICMJE (all authors have made substantial contributions to the conception, design, conduct of the study, and preparation of the manuscript, have read and approved the final version for publication).
References Comparison of hemodynamic changes and their management following subarachnoid block between normotensive and preeclamptic women undergoing cesarean section
- Cook TM, Counsell D, Wildsmith JA, et al. Major complications of central neuraxial block: report on the Third National Audit Project of the Royal College of Anaesthetists. Br J Anaesth. 2009;102(2):179-190. DOI: 10.1093/bja/aen360
- Rodgers A, Walker N, Schug S, et al. Reduction of postoperative mortality and morbidity with epidural or spinal anaesthesia: results from overview of randomised trials. BMJ. 2000;321(7275):1493. DOI: 10.1136/bmj.321.7275.1493
- Mohammed EL, El Shal SM. Efficacy of different size Quincke spinal needles in reduction of incidence of Post-Dural Puncture Headache (PDPH) in Caesarean Section (CS). Randomized controlled study. Egyptian J Anaesth. 2017;33:53-8.
- Pritchard JA, MacDonald PC. Hypertensive disorders in pregnancy. In: Pritchard JA, Macdonald PC, editors. Williams Obstetrics. 15 th ed. New York: Appleton Century Crofts; 1976. p. 551-812.
- Saha D, Ghosh S, Bhattacharyya S, et al. Comparison of hemodynamic response and vasopressor requirement following spinal anaesthesia between normotensive and severe preeclamptic women undergoing caesarean section: A prospective study. J Obstet Anaesth Crit Care. 2013;3:23-26. DOI: 10.4103/2249-4472.114286
- Chaudhary S, Salhotra R. Subarachnoid block for caesarean section in severe preeclampsia. J Anaesthesiol Clin Pharmacol. 2011;27(2):169-173. DOI: 10.4103/0970-9185.81821
- Mitra M, Basu D, Ganguly T, et al. Comparison of the Hemodynamic Alterations in Normotensive and Preeclamptic Pregnant Woman Posted for Cesarean Section under Subarachnoid Block. J Cardiovasc Dis Diagn. 2016;4: 242:1-7.
- Gofton EN, Capewell V, Natale R, Gratton RJ. Obstetrical intervention rates and maternal and neonatal outcomes of women with gestational hypertension. Am J Obstet Gynecol. 2001;185(4):798-803. DOI: 10.1067/mob.2001.117314
- Terrone DA, Isler CM, May WL, et al. Cardiopulmonary morbidity as a complication of severe preeclampsia HELLP syndrome. J Perinatol. 2000;20(2):78-81. DOI: 10.1038/sj.jp.7200315
- Tihtonen K, Kööbi T, Yli-Hankala A, et al. Maternal haemodynamics in pre-eclampsia compared with normal pregnancy during caesarean delivery. BJOG. 2006;113(6):657-663. DOI: 10.1111/j.1471-0528.2006.00931.x
- Kinzhalova SV, Makarov RA, Davydova NS. Hemodynamic effects of spinal anaesthesia during caesarian section in pregnant women with hypertensive disorders. Anesteziol Reanimatol. 2014;(3):25-29.
- Hurley RJ, Lambert DH. Continuous spinal anesthesia with a microcatheter technique: preliminary experience. Anesth Analg. 1990;70(1):97-102. DOI: 10.1213/00000539-199001000-00017
- Hood DD, Curry R. Spinal versus epidural anesthesia for cesarean section in severely preeclamptic patients: a retrospective survey. Anesthesiology. 1999;90(5):1276-1282. DOI: 10.1097/00000542-199905000-00009
- Sharwood-Smith G, Clark V, Watson E. Regional anaesthesia for caesarean section in severe preeclampsia: spinal anaesthesia is the preferred choice. Int J Obstet Anesth. 1999;8(2):85-89. DOI: 10.1016/s0959-289x(99)80003-x
- Hawkins JL, Koonin LM, Palmer SK, Gibbs CP. Anesthesia-related deaths during obstetric delivery in the United States, 1979-1990. Anesthesiology. 1997;86(2):277-284. DOI: 10.1097/00000542-199702000-00002
- Hawkins JL, Chang J, Palmer SK, et al. Anesthesia-related maternal mortality in the United States: 1979-2002. Obstet Gynecol. 2011;117(1):69-74. DOI: 10.1097/AOG.0b013e31820093a9
- Bromage PR. Epidural Analgesia. Philadelphia: WB Saunders; 1978.
- Aya AGM, Mangin R, Vialles N, et al. Patients with severe preeclampsia experience less hypotension during spinal anesthesia for elective cesarean delivery than healthy parturients: a prospective cohort comparison. Anesth Analg. 2003;97(3):867-872. DOI: 10.1213/01.ANE.0000073610.23885.F2
- Dyer RA, Piercy JL, Reed AR, et al. Hemodynamic changes associated with spinal anesthesia for cesarean delivery in severe preeclampsia. Anesthesiology. 2008;108(5):802-811. DOI: 10.1097/01.anes.0000311153.84687.c7
- Aya AGM, Vialles N, Tanoubi I, et al. Spinal anesthesia-induced hypotension: a risk comparison between patients with severe preeclampsia and healthy women undergoing preterm cesarean delivery. Anesth Analg. 2005;101(3):869-875. DOI: 10.1213/01.ANE.0000175229.98493.2B
- Visalyaputra S, Rodanant O, Somboonviboon W, et al. Spinal versus epidural anesthesia for cesarean delivery in severe preeclampsia: a prospective randomized, multicenter study. Anesth Analg. 2005;101(3):862-868. DOI: 10.1213/01.ANE.0000160535.95678.34


